---
# How HBOT Calms Autoimmune Flares: What the Science Says
**URL:** https://mdhyperbaric.com/blog/how-hbot-calms-autoimmune-flares
Date: 2026-04-08
Author: Jeff Lentz
Post Type: post
Summary: Autoimmune flares can feel unpredictable, especially during seasonal transitions. This article breaks down the science behind hyperbaric oxygen therapy (HBOT) and how it may help regulate immune response, reduce inflammatory cytokines, and support recovery in conditions like rheumatoid arthritis, lupus, and multiple sclerosis.
Categories: Blog
Tags: autoimmune diseases
Featured Image: https://mdhyperbaric.com/wp-content/uploads/2026/04/Untitled-design-20.png
---
**Reviewed by: Elizabeth Chan, NP (Medical Director, MD Hyperbaric)**
If you live with an [**autoimmune condition**](https://mdhyperbaric.com/conditions/autoimmune-disease) like lupus, rheumatoid arthritis, multiple sclerosis, psoriasis, or Hashimoto's thyroiditis, you're familiar with the cycle: things feel manageable for a while, then a flare hits and everything changes. Your joints swell. Your energy tanks. Your skin flares up. And for a lot of people, spring is when it all gets worse.
But why does spring seem to bring on flares? And what can you do about it beyond adjusting medications and waiting it out?
**[Hyperbaric oxygen therapy (HBOT)](https://mdhyperbaric.com/what-is-hbot)** is showing real promise as a way to help manage autoimmune flares. In this post, we'll break down why spring is such a tough season for autoimmune conditions, how oxygen actually works to calm your immune system, and who's most likely to benefit.
## Why Spring Is So Hard on Autoimmune Conditions?
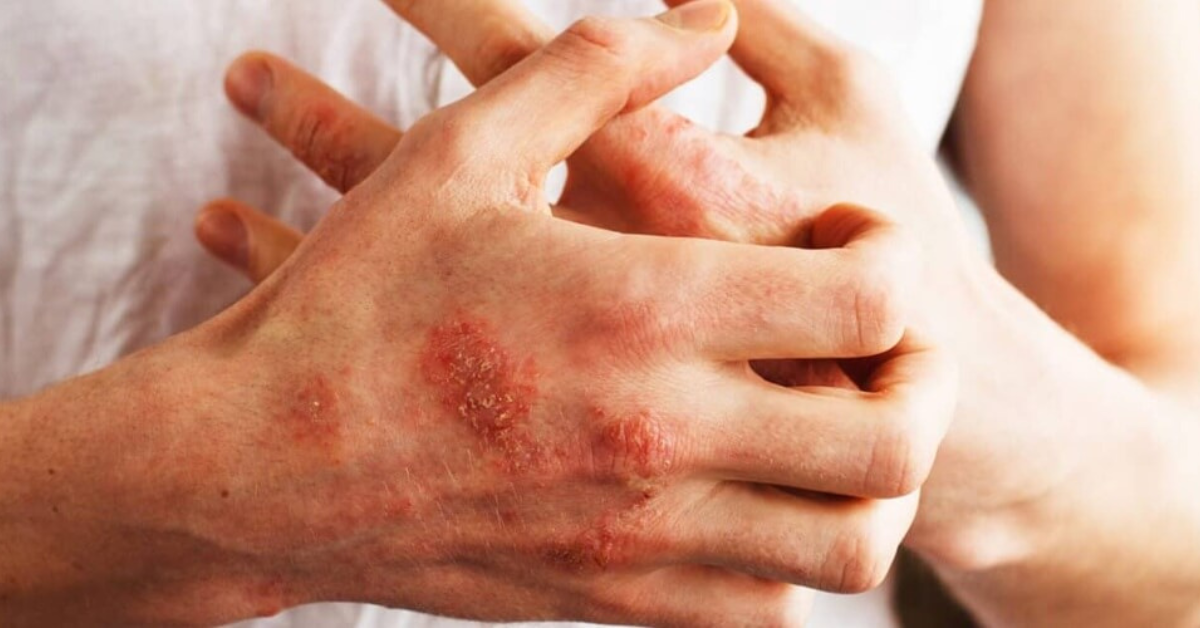
Spring is gorgeous, but if your immune system is already overactive, it can also throw your body off balance. A few things are happening at once.
For starters, the longer days shift your sleep-wake cycle, which affects cortisol, one of your body's natural tools for **[keeping inflammation in check](https://mdhyperbaric.com/blog/your-inflammation-survival-guide-how-hbot-supports-healing)**. Even small changes to your cortisol rhythm can make inflammation harder to control. Studies have confirmed that rheumatoid arthritis symptoms tend to get worse during seasonal transitions, especially in spring.[1]
Then there's pollen. For most people, pollen means sneezing. But if your immune system is already in overdrive, those allergens can kick off a bigger inflammatory reaction that spills over into your autoimmune symptoms. Your body gears up to fight pollen, and in the process, it cranks up the same pathways that are already attacking your own tissue.
On top of that, spring often brings changes in routine: different sleep patterns, more physical activity after a slow winter, shifts in diet. Any one of these can nudge your immune system in the wrong direction. Together, they can trigger a full-blown flare.
A 2019 study tracking over 12,000 rheumatoid arthritis patients found that flares in the small joints of the hands and feet were most common in spring, followed by winter.[2] A separate large-scale analysis backed this up, linking the spring peak to changes in how immune-related genes are expressed as the climate shifts.[3]
And here's one more factor: by the end of winter, many people's vitamin D levels have bottomed out. Vitamin D plays a key role in keeping your immune system balanced, and low levels have been linked to increased autoimmune activity in conditions like MS and lupus. So by the time spring rolls around, your body may already be running on empty.
## How Oxygen Helps Your Immune System Find Balance

To understand why HBOT helps with flares, it helps to understand a bit about how your immune system communicates.
Your body uses tiny messenger molecules called cytokines to coordinate its immune response. Think of them as signals that either turn inflammation up or turn it down. In autoimmune disease, the "turn it up" signals (like TNF-α and IL-6) overpower the "turn it down" signals (like IL-10). That imbalance is what drives the pain, swelling, and tissue damage you feel during a flare.
HBOT works by having you breathe pure oxygen in a pressurized chamber. Under that pressure, your blood absorbs far more oxygen than it normally would, up to 10 to 15 times the usual amount. That extra oxygen reaches deep into inflamed areas that your blood supply might be struggling to get to on its own.
Here's where it gets really interesting. A 2021 study found that HBOT significantly lowered the pro-inflammatory signals (the ones that drive flares) while boosting the anti-inflammatory signals that help calm things down.[4] A 2022 study confirmed similar effects on immune markers and oxidative stress.[5]
A major 2024 review looking at 780 patients found the same pattern: HBOT consistently increased the calming signals (IL-10) while reducing the inflammatory ones (TNF-α and IL-6).[6]
HBOT also supports your immune system in other ways. It helps activate regulatory T-cells, which are basically your body's peacekeepers, the cells that tell the immune system to stand down when it's attacking healthy tissue. It boosts your body's natural antioxidant defenses. And it makes it harder for inflammatory cells to pile into your tissues and cause damage.[7]
The bottom line: HBOT doesn't shut your immune system off the way some medications do. It helps bring it back into balance.
## What Treatment Looks Like
At MD Hyperbaric, we build a **[treatment plan around your specific condition and symptoms](https://mdhyperbaric.com/blog/why-hbot-works-best-in-series-understanding-treatment-protocols-and-how-the-number-of-sessions-impacts-your-results?utm_source=demand_gen&utm_medium=cpc&utm_campaign=farmington&utm_content=brand_awareness&utm_term=120235819584010165&fbclid=fbclid&gclid=CjwKCAiA-__MBhAKEiwASBmsBEGm3gkzLy3CTMKNWR6XoFOH0E759XX29N8A5hQGoIAJjuWuY8QHDRoCB_sQAvD_BwE)**. While every case is different, most autoimmune patients go through 20 to 40 sessions, each lasting about 60 to 90 minutes.
A lot of patients start feeling a difference within the first 10 sessions: less joint stiffness, more energy, better sleep, and a general feeling that the flare is losing steam. Those early changes reflect the shift in inflammatory signals and improved oxygen delivery that starts within the first few treatments.
The full benefits tend to build over the course of treatment. The improvements in immune balance, antioxidant capacity, and tissue repair are cumulative, which is why sticking with the full course matters.
## Who Benefits Most?
HBOT isn't meant to replace your doctor or your medications. It works alongside them, targeting the underlying inflammation that fuels flares.
You might be a great fit for HBOT if you keep having flares even though you're on standard treatment, if your symptoms tend to get worse with the seasons (especially spring and fall), if autoimmune fatigue is dragging you down and nothing seems to help, if you have a condition with a strong inflammatory component like RA, lupus, MS, psoriatic arthritis, or ankylosing spondylitis, or if you're looking for something non-pharmaceutical to add to your care plan.
HBOT has a strong safety track record in clinical settings. Side effects are uncommon and usually minor, things like temporary ear pressure or feeling a bit tired after a session.
## The Bottom Line
You don't have to just ride out autoimmune flares and hope for the best. The research is showing that HBOT can meaningfully shift the immune imbalance that drives these episodes. It calms the inflammatory signals, supports your body's built-in peacekeeping cells, and delivers healing oxygen to the tissues that need it most.
If spring has always been a rough season for your autoimmune health, this might be the year to try something different.
**References & Supporting Research**
[1] Strusberg I, et al. "Influence of weather conditions on rheumatic pain." Journal of Rheumatology. 2002;29(2):335-338.
[2] Iikuni N, et al. "Influence of seasonal changes on disease activity and distribution of affected joints in rheumatoid arthritis." BMC Musculoskeletal Disorders. 2019;20:38.
[3] Ryu HJ, et al. "Seasonal exacerbation of rheumatoid arthritis detected by big claims data analysis." Modern Rheumatology. 2022;32(5):887-893.
[4] Liang F, et al. "Hyperbaric oxygen therapy alleviates autoimmune encephalomyelitis via the reduction of IL-17a and GM-CSF production." BMC Neuroscience. 2021;22:43. PMID: 34440146.
[5] Heyboer M, et al. "The effect of hyperbaric oxygen therapy on markers of oxidative stress and the immune response in healthy volunteers." Frontiers in Physiology. 2022;13:826163.
[6] Labrousse-Arias D, et al. "New insights of hyperbaric oxygen therapy: focus on inflammatory bowel disease." Precision Clinical Medicine. 2024;7(1):pbae001.
[7] Luongo C, et al. "Hyperbaric oxygen treatment is associated with a decrease in cytokine levels in patients with necrotizing soft-tissue infection." Undersea & Hyperbaric Medicine. 2021;48(2):147-156.
## Reviewed by
**Elizabeth Chan, NP** (Medical Director, MD Hyperbaric)
Elizabeth Chan, NP, serves as Medical Director at MD Hyperbaric and reviews educational content for clinical accuracy, patient safety, and clarity. She supports evidence-informed care planning for people exploring hyperbaric oxygen therapy for recovery, neurological symptoms, and wellness goals.

*Disclaimer: This article is for informational purposes only and does not constitute medical or insurance advice. Please consult a qualified healthcare provider for personal recommendations and check with your insurance company for current policy details.*
---
## Categories
- Blog
---
## Navigation
- [MD Hyperbaric](https://mdhyperbaric.com/)
## Tags
- autoimmune diseases
---
## Footer Links
- [SKT Doctor](https://www.sktthemes.org/shop/free-medical-clinic-wordpress-theme/)